Have you ever had a nagging pain in your jaw that just won’t quit? Or maybe a clicking sound every time you chew?
You’re not alone.
Many people face issues with their temporomandibular joint (TMJ), and finding the right treatment can be life-changing.
At South Calgary Oral Surgery, we specialize in providing top-notch dental TMJ alignment treatment near you, helping you regain comfort and functionality in your jaw.
We offer TMJ pain relief through a variety of non-invasive and therapeutic options tailored to your needs.
A proper TMJ diagnosis is crucial for effective treatment.
Introduction
Imagine your jaw as a finely tuned orchestra, with each movement perfectly synchronized.
But what happens when one instrument is out of tune?
The whole performance suffers. Similarly, when your TMJ is misaligned, it can throw off the harmony of your mouth, leading to pain and discomfort.
In this blog, we’ll explore when dental TMJ alignment treatment is needed, why you should consider it, what the treatment entails, and why South Calgary Oral Surgery is your go-to place for TMJ alignment needs.
When is Dental TMJ Alignment Treatment Needed?
Identifying the Signs of Temporomandibular Joint Disorder
You might be wondering if your jaw pain warrants a visit to the oral surgeon. TMJ disorders can present themselves in various ways, making it crucial to recognize the symptoms early. Common signs include:
Chronic jaw pain or tenderness
Difficulty chewing or speaking
Clicking or popping sounds in the jaw
Limited range of motion in the jaw
Frequent headaches or earaches
Ear pain
Shoulder pain
These symptoms can significantly impact your daily life, making it vital to seek dental TMJ alignment treatment early on. Dr. Miller Smith, a renowned oral surgeon at South Calgary Oral Surgery, explains, “Early intervention is key in managing TMJ disorders effectively. Ignoring the symptoms can lead to more severe complications over time.”
Understanding the Causes
TMJ disorders can stem from various factors, including:
Arthritis: This can wear down the cartilage in the TMJ, leading to pain and stiffness.
Jaw injury: Trauma to the jaw can cause misalignment or damage to the TMJ.
Chronic teeth grinding (bruxism): Grinding your teeth can put excessive pressure on the TMJ and jaw joints, potentially leading to TMJ disorder.
Misalignment of teeth or jaw: A misaligned bite can strain the TMJ, causing discomfort.
Knowing the underlying cause can help tailor the treatment to address the specific issue, providing more effective relief.

The Importance of Timely Treatment
Delaying treatment can exacerbate the problem, leading to chronic pain and potential damage to the jaw joint.
Studies show that early intervention can prevent long-term complications and improve the quality of life for patients suffering from TMJ disorders.
According to a report by the National Institute of Dental and Craniofacial Research, approximately 10% of Canadians suffer from TMJ disorders, highlighting the prevalence and need for timely treatment.
The Connection Between TMJ Disorders and Overall Health
TMJ disorders don’t just affect your jaw; they can impact your overall health. Chronic pain can lead to sleep disturbances, stress, and even depression.
Additionally, the constant strain on your jaw muscles can cause tension headaches and neck pain.
Addressing TMJ disorders promptly can help improve your overall well-being, allowing you to live a more comfortable and pain-free life.
Why Consider Dental TMJ Alignment Treatment Near Me?
Enhanced Quality of Life
Living with TMJ disorders can be a daily struggle, affecting everything from eating to speaking.
Dental TMJ alignment treatment can significantly improve your quality of life by providing TMJ pain relief and restoring normal jaw function.
Imagine being able to enjoy your favorite foods again without discomfort or speaking clearly without hesitation.
Preventing Further Complications
Untreated TMJ disorders can lead to more severe issues, such as chronic pain, arthritis in the jaw joint, and even damage to your teeth due to grinding.
Orthodontic treatment, including bite splints and adjustments to existing restorations, can also be a preventive measure for TMJ complications.
By seeking dental TMJ alignment treatment near you, you can prevent these complications and maintain optimal oral health.
Personalized Treatment Plans
At South Calgary Oral Surgery, we understand that every patient is unique. Our team of oral surgeons will work with you to develop a personalized treatment plan tailored to your specific needs.
Dr. Brad Fisher emphasizes, “A one-size-fits-all approach doesn’t work for TMJ disorders. We take the time to understand each patient’s condition and create a treatment plan that addresses their specific needs.”

Cost-Effective Solution
Investing in dental TMJ alignment treatment near you can save you money in the long run. Untreated TMJ disorders can lead to more severe dental issues that require costly treatments.
By addressing the problem early, you can avoid these additional expenses and enjoy a healthier, pain-free life.
Positive Impact on Mental Health and TMJ Pain
Living with chronic pain can take a toll on your mental health.
Studies have shown that chronic pain is closely linked to anxiety and depression.
By seeking treatment for your TMJ disorder, you can alleviate this pain and improve your overall mental well-being.
At South Calgary Oral Surgery, we believe in a mentally aware approach to health, addressing both the physical and emotional aspects of TMJ disorders.
The Role of an Oral Surgeon in TMJ Treatment
Oral surgeons play a crucial role in diagnosing and treating TMJ disorders.
Their specialized training and expertise allow them to accurately identify the root cause of the problem and recommend the most effective treatment options.
At South Calgary Oral Surgery, our team of experienced oral surgeons is dedicated to providing comprehensive care for patients with TMJ disorders.
What Does Dental TMJ Alignment Treatment Entail?

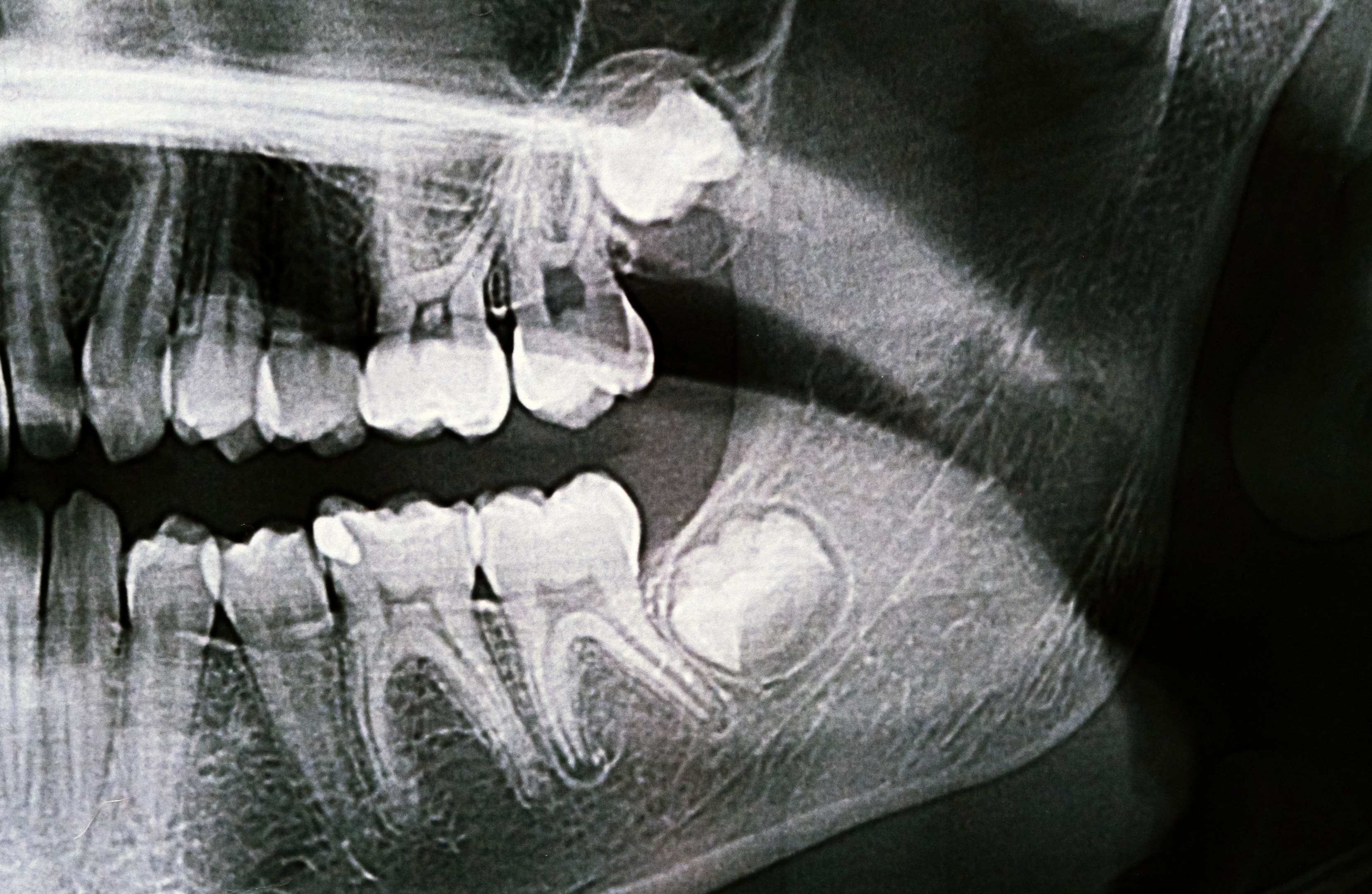
Comprehensive Examination
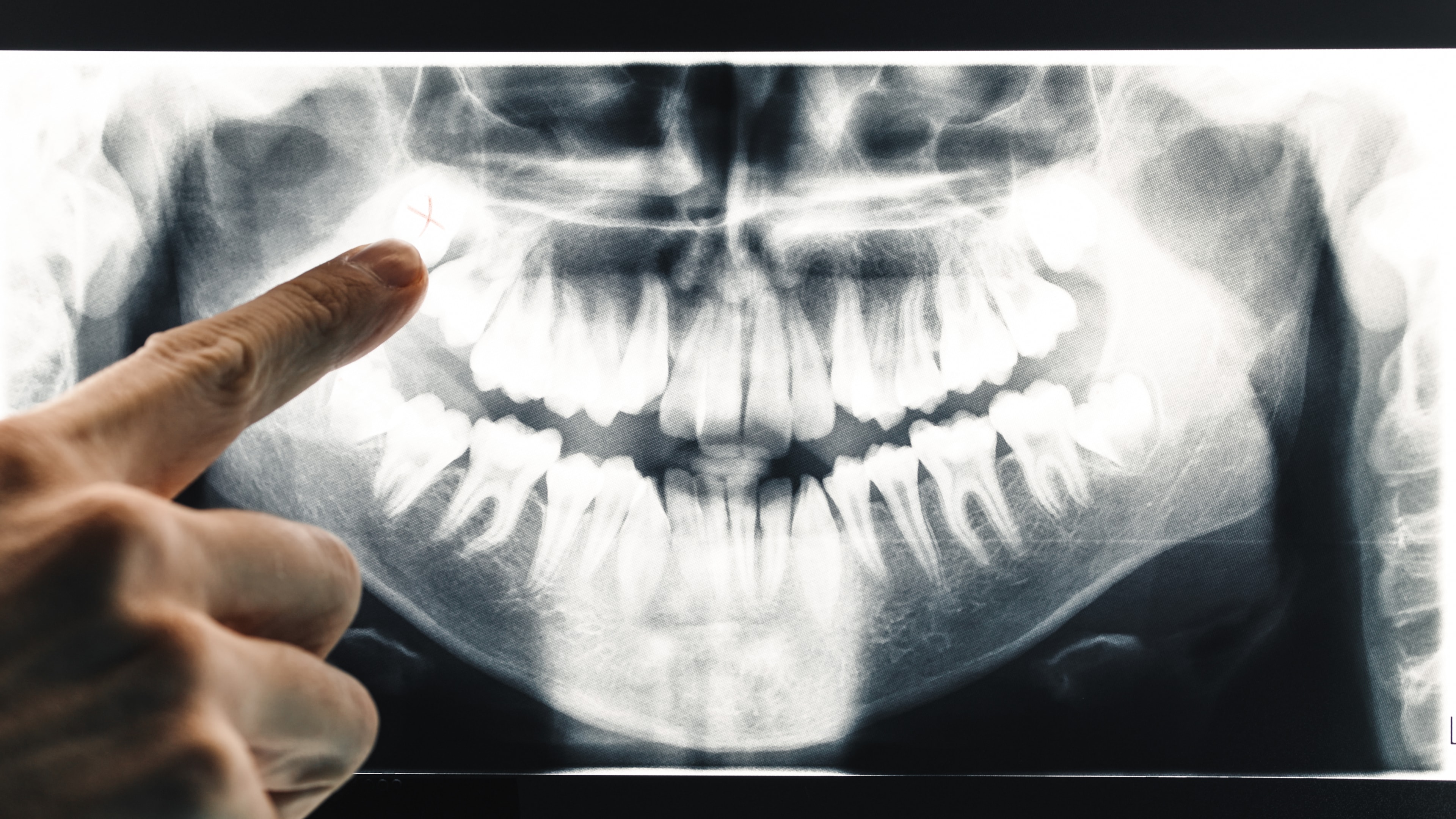
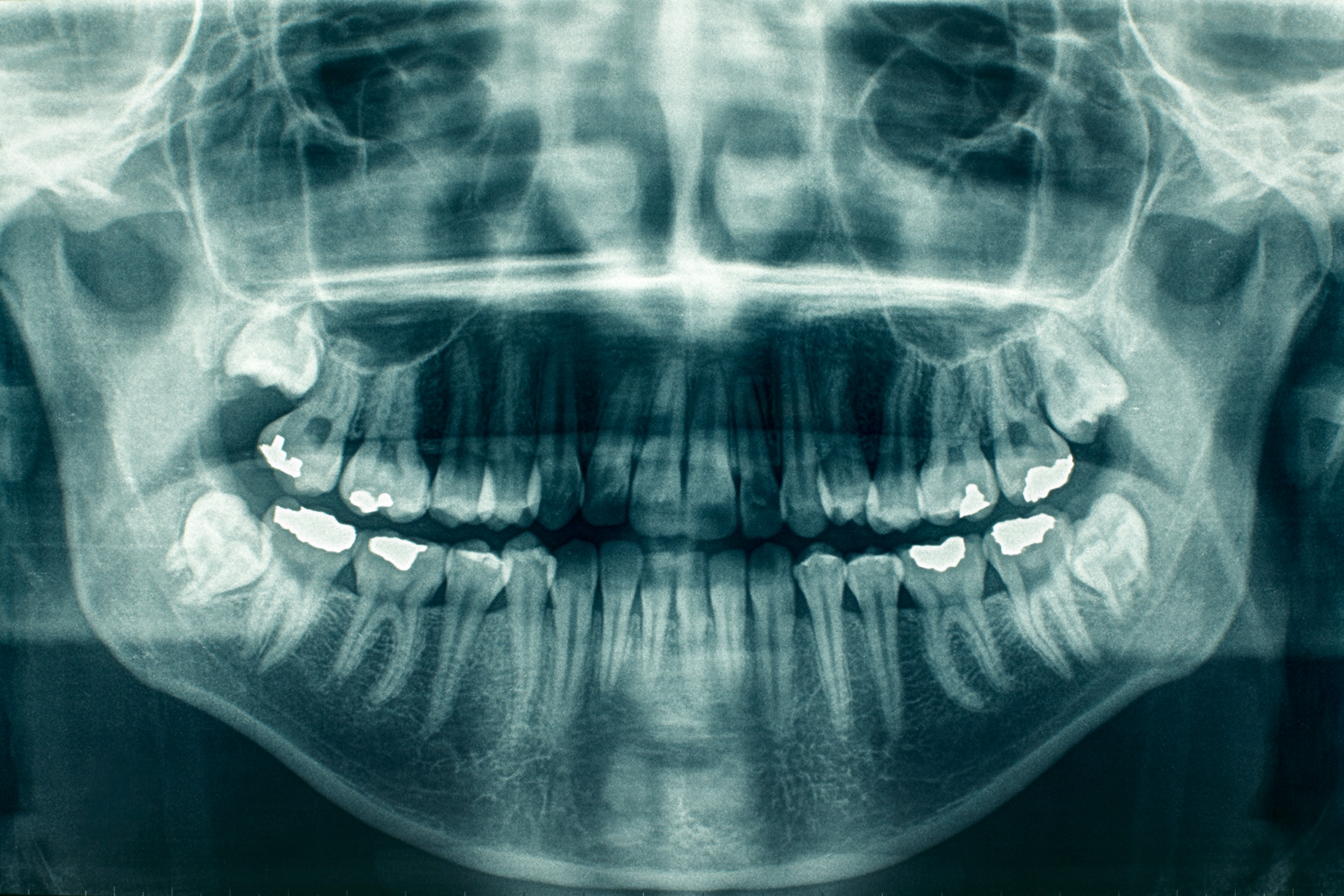
The first step in the treatment process is a comprehensive examination to ensure a proper TMJ diagnosis.
This includes a detailed medical history, a physical examination of the jaw, and imaging studies such as X-rays or MRI.
This thorough assessment helps us understand the extent of the disorder and plan the most effective treatment.
Non-Surgical TMJ Treatment
In many cases, non-surgical TMJ treatments can effectively manage TMJ disorders. TMJ pain relief is a primary goal of these treatments. These may include:
Medications: Pain relievers, anti-inflammatories, or muscle relaxants to alleviate symptoms.
Physical Therapy: Exercises to strengthen the jaw muscles and improve mobility.
Oral Appliances: Custom-made splints or mouthguards to prevent teeth grinding and reduce pressure on the jaw joint.
Medications and Their Role
Medications can play a significant role in managing TMJ disorders.
Over-the-counter pain relievers and anti-inflammatories can provide relief from mild to moderate pain.
In more severe cases, your oral surgeon may prescribe stronger pain medications or muscle relaxants to help alleviate muscle spasms and discomfort.
Physical Therapy for TMJ Disorders
Physical therapy is a non-invasive treatment option that can be highly effective in managing TMJ disorders.
It can also help alleviate symptoms such as shoulder pain associated with TMJ disorders. A physical therapist can teach you specific exercises to strengthen the muscles around your jaw, improve your range of motion, and reduce pain.
Techniques such as ultrasound therapy, heat and cold therapy, and manual therapy can also be used to alleviate symptoms.
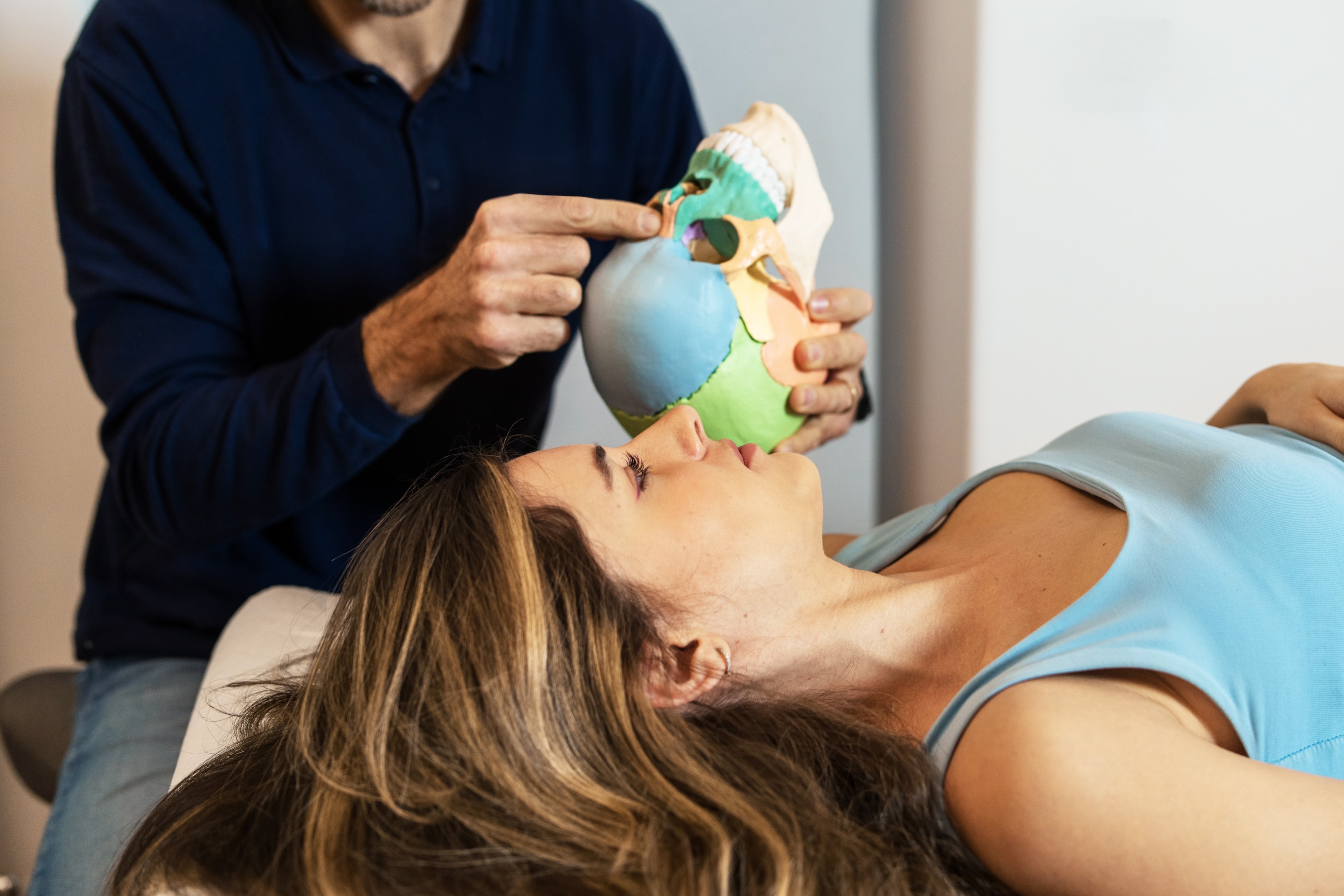
The Benefits of Oral Appliances
Oral appliances, such as splints or mouthguards, can be custom-made to fit your mouth and help alleviate the symptoms of TMJ disorders.
These devices work by redistributing the forces in your mouth, reducing the pressure on your TMJ, and preventing teeth grinding.
Wearing an oral appliance at night can significantly reduce the strain on your jaw joints and improve your symptoms.
Surgical Interventions
For more severe cases, surgical intervention and TMJ treatments may be necessary. Our skilled oral surgeons at South Calgary Oral Surgery are experienced in performing various surgical procedures, including:
Arthrocentesis: A minimally invasive procedure to flush out the joint and reduce inflammation.
Arthroscopy: Using a small camera and instruments to repair or remove damaged tissue.
Open-Joint Surgery: In rare cases, open surgery may be required to repair or replace the jaw joint.
Understanding Arthrocentesis
Arthrocentesis is a minimally invasive procedure that involves inserting small needles into the TMJ to wash out the joint.
This can help reduce inflammation and improve mobility. Arthrocentesis is typically performed under local anesthesia and can provide significant relief for patients with mild to moderate TMJ disorders.
The Role of Arthroscopy
Arthroscopy is a more advanced procedure that involves inserting a small camera (arthroscope) into the TMJ to diagnose and treat the disorder with great precision.
The camera allows the oral surgeon to see inside the joint and make precise repairs using small instruments. Arthroscopy is less invasive than open-joint surgery and typically has a shorter recovery time.
When Open-Joint Surgery is Necessary
In rare cases, open-joint surgery may be required to repair or replace the TMJ.
This procedure is typically reserved for severe cases that do not respond to other treatments. Open-joint surgery involves making an incision in front of the ear to access the joint and make necessary repairs.
While this procedure is more invasive, it can provide significant relief for patients with advanced TMJ disorders.
Post-Treatment Care
After the treatment, follow-up care is crucial to ensure a successful recovery.
This may include regular check-ups, physical therapy, and lifestyle modifications to prevent recurrence.
Our team is committed to providing ongoing support to help you achieve and maintain optimal jaw health.

Lifestyle Modifications for TMJ Management
Making certain lifestyle changes can help manage the symptoms of TMJ disorders and prevent recurrence. These may include:
Stress Management: Practicing stress-reducing techniques such as meditation, yoga, or deep breathing exercises can help reduce tension in your jaw muscles.
Diet Modifications: Eating a soft diet and avoiding hard or chewy foods can reduce strain on the TMJ.
Posture Improvement: Maintaining good posture can help reduce the strain on your jaw and neck muscles.
The Importance of Follow-Up Care
Regular follow-up appointments with your oral surgeon are essential to monitor your progress and make any necessary adjustments to your treatment plan.
These appointments allow your surgeon to assess your recovery, address any concerns, and provide additional recommendations for managing your TMJ disorder.
Why Choose South Calgary Oral Surgery for Your TMJ Alignment Needs?

Expertise and Experience
Our team of oral surgeons at South Calgary Oral Surgery has extensive experience in diagnosing and treating TMJ disorders, offering expert TMJ treatment in Calgary.
With years of specialized training and a deep understanding of the complexities of the jaw joint, we are well-equipped to provide the highest level of care.
State-of-the-Art Technology
We utilize the latest technology and techniques to ensure accurate diagnosis and effective treatment.
Our state-of-the-art facility is equipped with advanced imaging and surgical equipment, allowing us to deliver precise and minimally invasive care.
Patient-Centered Approach
At South Calgary Oral Surgery, we prioritize our patients’ comfort and satisfaction.
From the moment you walk through our doors, you will be treated with compassion and respect.
Our team takes the time to listen to your concerns, answer your questions, and involve you in every step of the treatment process.
Convenient Location
Located in the heart of Calgary, AB, our practice is easily accessible to residents of SE and SW Calgary and surrounding communities. Finding “dental TMJ alignment treatment near me” has never been easier.
Positive Patient Outcomes
We take pride in the positive outcomes we achieve for our patients. Many of our patients have experienced significant relief from their TMJ pain and improved their quality of life through our treatments. Our commitment to excellence is reflected in the numerous positive reviews and testimonials from satisfied patients.
Meet Our Team
Our team of oral surgeons, including Dr. Miller Smith, Dr. Graham Cobb, and Dr. Brett Habijanac, bring a wealth of knowledge and expertise to the practice. Each member of our team is dedicated to providing the highest standard of care and ensuring the best possible outcomes for our patients.
The Benefits of Choosing a Specialized Practice
Choosing a specialized practice like South Calgary Oral Surgery for your TMJ alignment needs offers several advantages:
Expertise: Our oral surgeons have specialized training and experience in diagnosing and treating TMJ disorders.
Comprehensive Care: We provide a full range of treatment options, from non-surgical therapies to advanced surgical procedures.
Personalized Approach: We take the time to understand each patient’s unique needs and develop a customized treatment plan.
Advanced Technology: Our state-of-the-art facility is equipped with the latest technology to ensure accurate diagnosis and effective treatment.
Ongoing Support: We are committed to providing ongoing support and follow-up care to ensure the best possible outcomes for our patients.
Conclusion
Living with TMJ disorders can be challenging, but effective treatment is available. By seeking dental TMJ alignment treatment near you, you can alleviate pain, improve jaw function, and prevent further complications.
At South Calgary Oral Surgery, we are committed to providing exceptional care tailored to your specific needs.
Don’t let TMJ disorders hold you back—take the first step towards a pain-free life today. Contact us to schedule a consultation and discover how our expert team can help you achieve optimal jaw health.

In summary, recognizing the signs of TMJ disorders early and seeking timely treatment can significantly improve your quality of life. At South Calgary Oral Surgery, our team of experienced oral surgeons is dedicated to providing comprehensive, patient-centered care.
With our state-of-the-art technology, personalized treatment plans, and commitment to positive patient outcomes, we are the top choice for “dental TMJ alignment treatment near me”.
Remember, taking action today can prevent further complications and help you live a healthier, more comfortable life. So, why wait? Reach out to us and start your journey to optimal jaw health today.